Bursitis Of The Foot Remedy
Calcaneal bursitis is seen somewhat frequently, particularly if the clinician has a predominantly musculoskeletal practice. No mortality is associated with calcaneal bursitis. Morbidity is associated with progressive pain and limping (antalgic gait) in patients who have not received adequate treatment. If chronic inflammation also affects the distal Achilles tendon, rupture of the tendon may occur. No race predilection has been documented. Calcaneal bursitis is observed in men and women. However, some increased risk may be incurred by women who wear high-heeled shoes. Calcaneal bursitis is commonly observed in middle-aged and elderly persons, the condition is also seen in athletes of all ages.Bursitis is a painful swelling of a small sac of fluid called a bursa. Bursae (plural of bursa) cushion and lubricate areas where tendons, ligaments, skin, muscles, or bones rub against each other. People who repeat the same movement over and over or who put continued pressure on a joint in their jobs, sports, or daily activities have a greater chance of getting bursitis.
Causes
Although rare, bursitis also may be caused by an infection, known as septic bursitis. This is a serious medical condition that requires antibiotics to treat the infection and prevent its spread to other points in the body or the bloodstream. Septic bursitis may cause the back of the ankle to become red or hot. The person may also get the chills or fever and may feel sick and tired. Typically this type of bursitis would be suspected if there has been any history of an open wound in the area, such as a blister.
Symptoms
Symptoms of bursitis include pain in the heel, especially with walking, running, or when the area is touched. The skin over the back of the heel may be red and warm, and the pain may be worse with attempted toe rise (standing on tippy-toes).
Diagnosis
When you suspect you have retrocalcaneal bursitis, your foot doctor will begin by taking a complete history of the condition. A physical exam will also be performed. X-rays are usually taken on the first visit as well to determine the shape of the heel bone, joint alignment in the rearfoot, and to look for calcium deposits in the Achilles tendon. The history, exam and x-rays may sufficient for your foot surgeon to get an idea of the treatment that will be required. In some cases, it may be necessary to get an ultrasound or MRI to further evaluate the Achilles tendon or its associated bursa. While calcium deposits can show up on xray, the inflammation in the tendon and bursa will show up much better on ultrasound and MRI. The results of these tests can usually be explained on the first visit. You can then have a full understanding of how the problem started, what you can do to treat prevent it from getting worse/ You will also know which treatment will be most helpful in making your heel pain go away.
Non Surgical Treatment
Surgery should always be the last option. We believe that biologic treatments that preserve normal anatomy are very helpful, particularly for runner, athletes, and active professionals with buy schedules. All non-surgical approaches attempt to calm down the inflammation of the bursa and Achilles tendon. They do not address the bony bump, but they can substantially reduce and shrink the inflamed soft tissue. Some non-surgical treatments include Oral Anti-inflammatory Medications. NSAID's (non-steroidal anti-inflammatory medications) such as Motrin, Aleve, and Steroids (like prednisone) may help control the pain and stop the inflammation. Topical Anti-inflammatory Medications. NSAID's in cream or lotion form may be applied directly to the inflamed area. With these, there is no concern for stomach upset or other problems associated with oral medication. Ice. Ice can applied be applied right to the red, inflamed area and help calm it down. Try applying a podiatrist-approved ice pack to the affected area for 20 minutes of each hour. Just make sure you don't put ice directly against the skin. Exercises. Stretching exercises may relieve some of the tension in the Achilles tendon that started the problem. If you have Equinus Deformity (or a tight heel cord) this is critical to prevent it from coming back again. Heel lifts. Heel lifts placed inside the shoe can decrease the pressure on the Achilles tendon. Remember, pressure and friction cause the bump to become inflamed. Heel pads. Placing gel padding to cushion the Achilles tendon (at the back of the heel) can also help reduce irritation from shoes. Shoe modification. Wearing open-backed shoes, or shoes that have soft backs. This will also help stop the irritation. Physical therapy. Physical therapy, such as ultrasound, massage and stretching can all reduce the inflammation without surgery. Orthotic devices. Custom arch supports known as foot orthotics control abnormal motion in the foot that can allow the heel to tilt over and rub against the heel counter. Orthotics can decrease symptoms and help prevent it from happening again. Immobilization. In some cases, a walking cast boot or plaster/fiberglass cast is necessary to take pressure off the bursa and tendon, while allowing the area to calm down. ESWT. Extra-corporeal Shock Wave Therapy uses high energy sound waves to break up diseased tissue in the bursa and Achilles tendon and stimulate your own bodies healing processes to repair the diseased area. It may be done in the office or in a an outpatient surgery center. There is no incision and no stitches with ESWT. PRP. Platelet Rich Plasma (PRP) is a therapeutic injection. A small sample of blood is drawn from the patient and the healing factors found in the platelets are concentrated in a centrifuge. By injecting the concentrated solution right into the damaged Achilles tendon, a powerful healing can be stimulated. This can be done in the office. No hospital or surgery required.
Surgical Treatment
Surgery is rarely done strictly for treatment of a bursitis. If any underlying cause is the reason, this may be addressed surgically. During surgery for other conditions, a bursa may be seen and removed surgically.
Hammer Toe Cure
 Overview
Overview
Hammer toe is most common in women, and a big part of this is poor shoe choices, which are a big factor in the development of many foot problems. Tight toe boxes and high heels are the biggest culprits. Genetics certainly plays a role in some cases of hammertoes, as does trauma, infection, arthritis, and certain neurological and muscle disorders. Most cases of contracted toes are associated with various biomechanical abnormalities in how a patient walks. This causes the muscles and tendons to be used excessively or improperly, which deforms the toes over time.
Causes
Hammer toe results from shoes that don't fit properly or a muscle imbalance, usually in combination with one or more other factors. Muscles work in pairs to straighten and bend the toes. If the toe is bent and held in one position long enough, the muscles tighten and cannot stretch out. Shoes that narrow toward the toe may make your forefoot look smaller. But they also push the smaller toes into a flexed (bent) position. The toes rub against the shoe, leading to the formation of corns and calluses, which further aggravate the condition. A higher heel forces the foot down and squishes the toes against the shoe, increasing the pressure and the hammertoe bend in the toe. Eventually, the toe muscles become unable to straighten the toe, even when there is no confining shoe.
 Symptoms
Symptoms
Symptoms may include pain in the affected toe or toes when you wear shoes, making it hard or painful to walk. A corn or callus on the top of the joint caused by rubbing against the shoe. Swelling and redness of the skin over the joint. Trouble finding comfortable shoes.
Diagnosis
A hammertoe is usually diagnosed with a physical inspection of your toe. Imaging tests, such as X-rays, may be ordered if you have had a bone, muscle, or ligament injury in your toe.
Non Surgical Treatment
Apply a commercial, nonmedicated hammertoe pad around the bony prominence of the hammertoe. This will decrease pressure on the area. Wear a shoe with a deep toe box. If the hammertoe becomes inflamed and painful, apply ice packs several times a day to reduce swelling. Avoid heels more than two inches tall. A loose-fitting pair of shoes can also help protect the foot while reducing pressure on the affected toe, making walking a little easier until a visit to your podiatrist can be arranged. It is important to remember that, while this treatment will make the hammertoe feel better, it does not cure the condition. A trip to the podiatric physician?s office will be necessary to repair the toe to allow for normal foot function. Avoid wearing shoes that are too tight or narrow. Children should have their shoes properly fitted on a regular basis, as their feet can often outgrow their shoes rapidly. See your podiatric physician if pain persists.
Surgical Treatment
In more advanced cases of hammer toe, or when the accompanying pain cannot be relieved by conservative treatment, surgery may be required. Different types of surgical procedures are performed to correct hammer toe, depending on the location and extent of the problem. Surgical treatment is generally effective for both flexible and fixed (rigid) forms of hammer toe. Recurrence following surgery may develop in persons with flexible hammer toe, particularly if they resume wearing poorly-fitted shoes after the deformity is corrected.
 Prevention
Prevention
The American Podiatric Medical Association offers the following tips for preventing foot pain. Don't ignore foot pain, it's not normal. Inspect feet regularly. Wash feet regularly, especially between the toes, and dry them completely. Trim toenails straight across, but not too short. Make sure shoes fit properly.
Hammer Toe Inherited Causes
 Overview
Overview
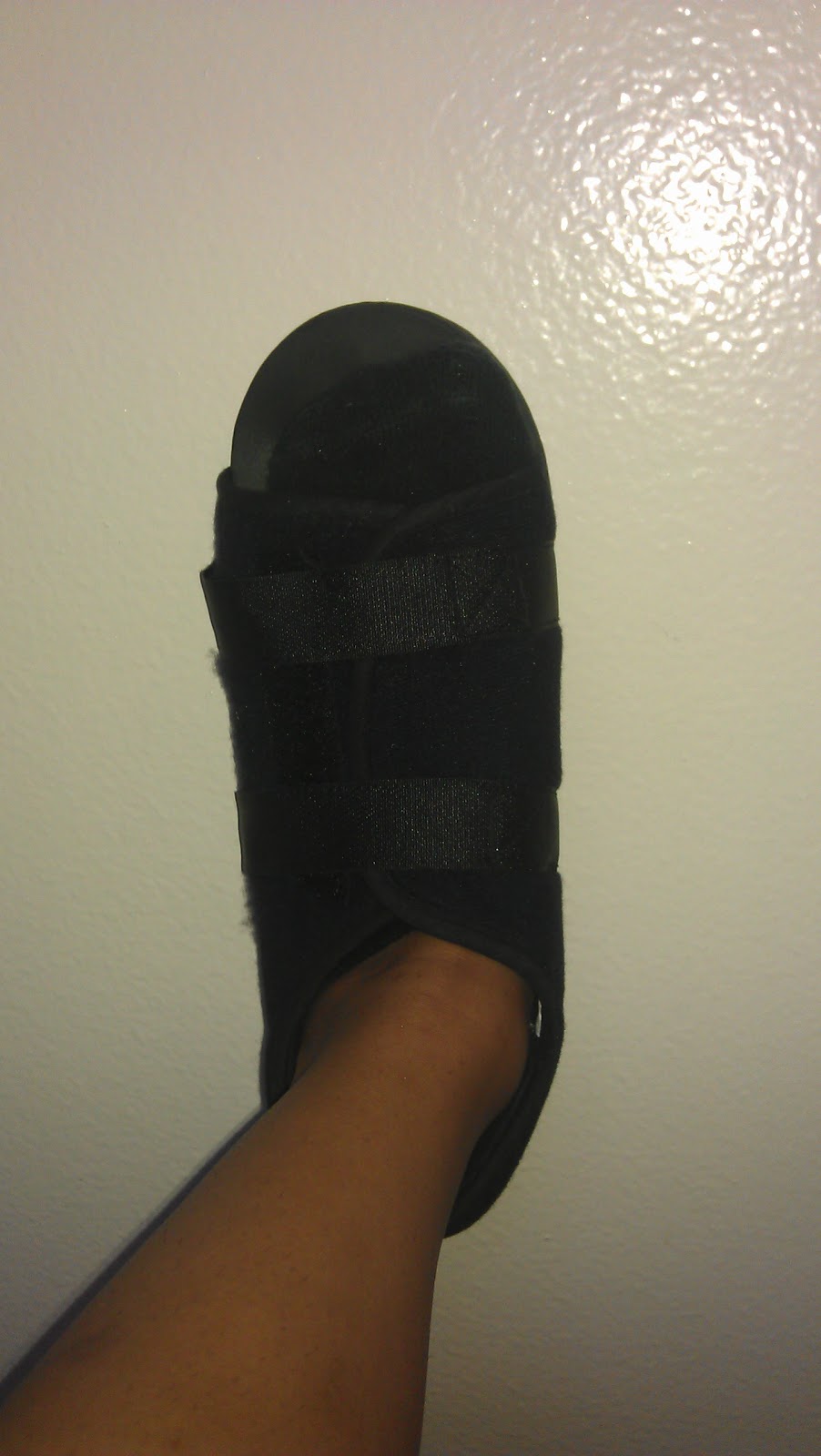
A Hammer toes is a contracture, or bending, of the toe at the first joint of the digit, called the proximal interphalangeal joint. This bending causes the toe to appear like an upside-down V when looked at from the side. Any toe can be involved, but the condition Hammer toe usually affects the second through fifth toes, known as the lesser digits. Hammer toes are more common in females than males.
Causes
Many people develop hammertoe because they wear shoes that are too tight. Shoes with narrow toe boxes squeeze the toes together, forcing some to bend. This causes the toe muscles to contract. If the toes are forced into this cramped position too often, the muscles may permanently tighten, preventing the toes from extending. Chronic hammertoe can also cause the long bones that connect the toes to the foot, called metatarsals, to move out of position. The misaligned metatarsal bones may pinch a nerve running between them, which can cause a type of nerve irritation called a neuroma.
 Symptoms
Symptoms
Pain on the bottom of your foot, especially under the ball of your foot, is one of the most common symptoms associated with hammertoes. Other common signs and symptoms of hammertoes include pain at the top of your bent toe from footwear pressure. Corns on the top of your bent toe. Redness and swelling in your affected area. Decreased joint range of motion in your affected toe joints.
Diagnosis
Your healthcare provider will examine your foot, checking for redness, swelling, corns, and calluses. Your provider will also measure the flexibility of your toes and test how much feeling you have in your toes. You may have blood tests to check for arthritis, diabetes, and infection.
Non Surgical Treatment
Inserts in your shoes can be used to help relieve pressure on the toes from the deformity. Splints/Straps. These can be used to help re-align and stretch your toes and correct the muscle imbalance and tendon shortening. One of the most common types are toe stretchers like the yogatoe. Chiropody. A chiropodist can remove calluses or corns, areas of hard skin that have formed to make the foot more comfortable.Steroid injections can help to reduce pain and inflammation.
Surgical Treatment
There are several surgical methods to correct a hammer toe. Your physician will decide which method will be most beneficial to you depending on the severity of your deformity, the direction the toe is deviating and the length of the affected toe. Some common surgical methods include. Arthroplasty. To promote straightening, half of the joint located directly underneath the crooked part of the toe is removed. Arthrodesis (fusion) To promote straightening, the joint directly underneath where the toe is crooked is completely removed. A wire or pin is inserted to aid healing. Tendon transfer. Performed alone or in combination with other procedures, a surgeon will take tendons from under the toe and ?re-route? them to the top of the toe to promote straightening. Basal phalangectomy. Performed to assist patients with severe stiffness, this procedure removes the base of the bone underneath the toe. Weil osteotomy. Performed to assist patients with severe stiffness, this procedure involves shortening the metatarsal bone and inserting surgical hardware to aid healing.
Bunions Reasons Warning Signs And Therapies
Overview
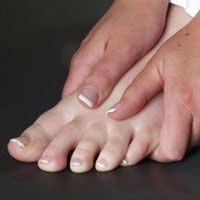 More than one-third of women in America have bunions, a common deformity often blamed on wearing tight, narrow shoes and high heels. Bunions may occur in families, but many are from wearing tight shoes, and nine out of 10 bunions happen to women. Too-tight shoes can also cause other disabling foot problems such as corns, calluses and hammer toes.
More than one-third of women in America have bunions, a common deformity often blamed on wearing tight, narrow shoes and high heels. Bunions may occur in families, but many are from wearing tight shoes, and nine out of 10 bunions happen to women. Too-tight shoes can also cause other disabling foot problems such as corns, calluses and hammer toes.
Causes
Perhaps the most frequent cause of bunion development is the wearing of shoes with tight, pointed toes, or with high heels that shift all of your body's weight onto your toes and also jam your toes into your shoes' toe boxes. It's estimated that more than 50 percent of women have bunions caused by high-heel shoes, and that nine out of 10 people who develop bunions are women. Bunions can also develop on your little toes, in which case they are called bunionettes or tailor's bunions.
Symptoms
Audible clicking (called ?crepitus?) and/or stiffness in the affected joint which indicates that the joint surfaces are rubbing together improperly. Inflammation, degeneration of the surfaces of the joint, deformity (including bone growth at the joint line and displacement of the toe) and ultimately, loss of range of motion in the joint. Pain at the side and top of the joint that worsens with walking and physical activity.
Diagnosis
Although bunions are usually obvious from the pain and unusual shape of the toe, further investigation is often advisable. Your doctor will usually send you for X-rays to determine the extent of the deformity. Blood tests may be advised to see if some type of arthritis could be causing the pain. Based on this evaluation, your doctor can determine whether you need orthopaedic shoes, medication, surgery or other treatment.
Non Surgical Treatment
Treatment may be surgical or non-surgical. The goal of non-surgical treatment is to relieve pressure on the foot and to prevent pressure sores and foot ulcers. This is accomplished by prescribing accommodative shoes with a wide toe box - sandals or extra depth shoes with soft moulded insoles. It may also be possible to relax the leather on shoes to make room for a bunion. 
Surgical Treatment
This involves surgically correcting the deformity and can involve a variety of different methods. However, outcomes can be variable. This is very dependant of the amount of damage to the joint and the procedure used to correct it. Removal of the bunion is performed using different methods that are out of the scope of this article. Unfortunately, bunions can recur following surgery, and even if it surgery is successful, around 30% of patients still report existing difficulties.
Prevention
Shop for shoes that possess a removable liner, or insole, and stand on the liner after you have removed it from your shoe. This is an effective method to see if your shoe is wide enough in the forefoot to accommodate your bunion. If your bunion and forefoot are wider than the insole, your shoe will squeeze and constrict your bunion and create the symptoms that define this health problem. The insole should also be wide enough to fully accommodate your big toe when it points outward, away from your other toes.
Over-Pronation Of The Feet What Are The Symptoms
Overpronation of the foot is not an injury itself but if you over pronate then you may be more susceptible to a number of sports injuries. It is often recognised as a flattening or rolling in of the foot but it is not quite as simple as that as the timing of when the foot rolls in is also important.

Causes
Over-pronation is very prominent in people who have flexible, flat feet. The framework of the foot begins to collapse, causing the foot to flatten and adding stress to other parts of the foot. As a result, over-pronation, often leads to Plantar Fasciitis, Heel Spurs, Metatarsalgia, Post-tib Tendonitis and/or Bunions. There are many causes of flat feet. Obesity, pregnancy or repetitive pounding on a hard surface can weaken the arch leading to over-pronation. Often people with flat feet do not experience discomfort immediately, and some never suffer from any discomfort at all. However, when symptoms develop and become painful, walking becomes awkward and causes increased strain on the feet and calves.
Symptoms
Symptoms can manifest in many different ways. The associated conditions depend on the individual lifestyle of each patient. Here is a list of some of the conditions associated with Over Pronation. Hallux Abducto Valgus (bunions). Hallux Rigidus (stiff 1st toe). Arch Pain. Heel Pain (plantar fascitis). Metatarsalgia (ball of the foot pain). Ankle sprains. Shin Splints. Achilles Tendonitis. Osteochondrosis. Knee Pain. Corns & Calluses. Flat Feet. Hammer Toes.
Diagnosis
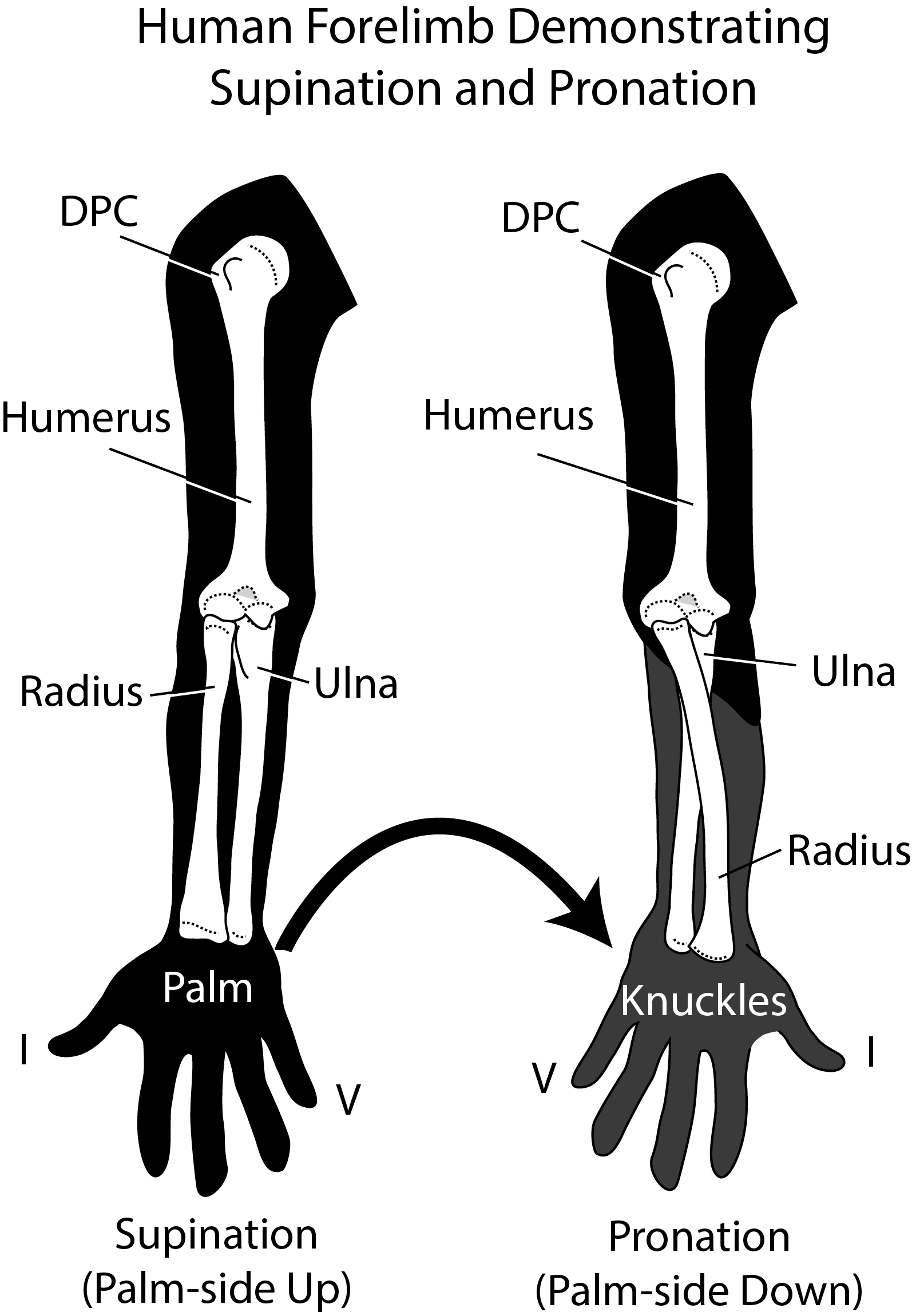
One of the easiest ways to determine if you overpronate is to look at the bottom of your shoes. Overpronation causes disproportionate wear on the inner side of the shoe. Another way to tell if you might overpronate is to have someone look at the back of your legs and feet, while you are standing. The Achilles tendon runs from the calf muscle to the heel bone, and is visible at the back of the ankle. Normally it runs in a straight line down to the heel. An indication of overpronation is if the tendon is angled to the outside of the foot, and the bone on the inner ankle appears to be more prominent than the outer anklebone. There might also be a bulge visible on the inside of the foot when standing normally. A third home diagnostic test is called the ?wet test?. Wet your foot and stand on a surface that will show an imprint, such as construction paper, or a sidewalk. You overpronate if the imprint shows a complete impression of your foot (as opposed to there being a space where your arch did not touch the ground).
Non Surgical Treatment
If you overpronate, you should talk with a foot and ankle specialist, especially if symptoms have not developed yet. Questions you may want to ask your doctor include what are the best running shoes on the market? Where can I find those shoes? If over-the-counter orthotics don?t work, how long should I wait before contacting you for custom-made orthotics? On my next visit, what type of diagnostic testing should I expect? If I limit the amount of time I spend running, will my overpronation symptoms disappear? What additional treatment options can we try?
Prevention
Wear supportive shoes. If we're talking runners you're going to fall in the camp of needing 'motion control' shoes or shoes built for 'moderate' or 'severe' pronators. There are many good brands of shoes out there. Don't just wear these running, the more often the better. Make slow changes. Sudden changes in your training will aggravate your feet more than typical. Make sure you slowly increase your running/walking distance, speed and even how often you go per week. Strengthen your feet. As part of your running/walking warm up or just as part of a nightly routine try a few simple exercises to strengthen your feet, start with just ten of each and slowly add more sets and intensity. Stand facing a mirror and practice raising your arch higher off the ground without lifting your toes. Sit with a towel under your feet, scrunch your toes and try to pull the towel in under your feet. Sitting again with feet on the ground lift your heels as high as you can, then raise and lower on to toe tips.
Physical Rehabilitation For Calcaneal Apophysitis
Severs disease is by far the most common cause of heel pain in young children, the condition commonly occurs in kids around the age of 10-15 years. Severs is a traction apophysitis in which inflammation of the calcaneal apophysis (growth plate) occurs as a result of overuse or micro trauma. As mentioned severs disease is caused by micro trauma and over use, this can include excessive foot pronation (foot rolling in), tight calf muscles, increase in sporting activities and inappropriate footwear. These all put extra sheering forces on the growth plate leading to aggravation and resultant pain. Signs and symptoms of this include pain on squeezing of the heel, absence of swelling and redness, child describing pain as a dull ache, limping and pain with increased activity.
Causes
The more active a child is then the greater the chance of suffering from Sever?s disease. Poor foot function such as flat feet causes the calf and Achilles to work harder and pull on the growth plate leading to Sever?s disease. Tight calves or Achilles is common in growing children and can increase tension on the growth plate.
Symptoms
Signs and symptoms of Sever?s disease include heel pain can be in one or both heels, and it can come and go over time. Many children walk or run with a limp, they may walk on their toes to avoid pressure on their heels. Heel pain may increase with running or jumping, wearing stiff, hard shoes (ex. soccer cleats, flip-flops) or walking barefoot. The pain may begin after increasing physical activity, such as trying a new sport or starting a new sports season.
Diagnosis
Children or adolescents who are experiencing pain and discomfort in their feet should be evaluated by a physician. In some cases, no imaging tests are needed to diagnose Sever?s disease. A podiatrist or other healthcare professional may choose to order an x-ray or imaging study, however, to ensure that there is no other cause for the pain, such as a fracture. Sever?s disease will not show any findings on an x-ray because it affects cartilage.
Non Surgical Treatment
Your podiatrist can help manage this condition by implementing a treatment program. This may incorporate one or all of the following. RI (Rest and Ice). Activity modification so child becomes pain free. Daily stretching routine. Heel raise within shoes to decrease pull on heel. Biomechanical abnormalities corrected (Orthotics). Strengthening of associated muscles. Footwear modification.
Achilles Tendon Rupture Thompson Testing
Overview
 The Achilles tendon is found in the back of the leg above the heel, and is the largest tendon in the body. It connects the calf muscles to the heel bone and is used when walking, running and jumping. A rupture of the tendon is a tearing and separation of the tendon fibers. When a rupture of the tendon occurs, the tendon can no longer perform its normal function. A common issue related to a tear is the inability to point your toe.
The Achilles tendon is found in the back of the leg above the heel, and is the largest tendon in the body. It connects the calf muscles to the heel bone and is used when walking, running and jumping. A rupture of the tendon is a tearing and separation of the tendon fibers. When a rupture of the tendon occurs, the tendon can no longer perform its normal function. A common issue related to a tear is the inability to point your toe.
Causes
Your Achilles tendon helps you point your foot downward, rise on your toes and push off your foot as you walk. You rely on it virtually every time you move your foot. Rupture usually occurs in the section of the tendon located within 2.5 inches (6 centimeters) of the point where it attaches to the heel bone. This section may be predisposed to rupture because it gets less blood flow, which may impair its ability to heal. Ruptures often are caused by a sudden increase in the amount of stress on your Achilles tendon. Common examples include increasing the intensity of sports participation, falling from a height, stepping into a hole.
Symptoms
Whereas calf strains and tendonitis may cause tightness or pain in the leg, Achilles tendon ruptures are typically accompanied by a popping sensation and noise at the time of the injury. In fact, some patients joke that the popping sound was loud enough to make them think they?d been shot. Seeing a board-certified orthopedic surgeon is the best way to determine whether you have suffered an Achilles tendon tear.
Diagnosis
A physician usually can make this diagnosis with a good physical examination and history. X-rays usually are not taken. A simple test of squeezing the calf muscles while lying on your stomach should indicate if the tendon is still connected (the foot should point). This test isolates the connection between the calf muscle and tendon and eliminates other tendons that may still allow weak movement. A word of caution, Achilles tendon rupture is often misdiagnosed as a strain or minor tendon injury. Swelling and the continuing ability to weakly point your toes can confuse the diagnosis. Ultrasound and MRI are tests that can assist in difficult diagnosis. Depending on the degree of injury, these tests can also assist in determining which treatment may be best.
Non Surgical Treatment
Once a diagnosis of Achilles tendon rupture has been confirmed, a referral to an orthopaedic specialist for treatment will be recommended. Treatment for an Achilles tendon rupture aims to facilitate the torn ends of the tendon healing back together again. Treatment may be non-surgical (conservative) or surgical. Factors such as the site and extent of the rupture, the time since the rupture occurred and the preferences of the specialist and patient will be considered when deciding which treatment will be undertaken. Some cases of rupture that have not responded well to non-surgical treatment may require surgery at a later stage. The doctor will immobilise the ankle in a cast or a special hinged splint (known as a ?moon boot?) with the foot in a toes-pointed position. The cast or splint will stay in place for 6 - 8 weeks. The cast will be checked and may be changed during this time. 
Surgical Treatment
Surgery is recommended to those who are young to middle-aged and active. The ruptured tendon is sewn together during surgery. This is an outpatient procedure. Afterward the leg is put into a splint cast or walking boot. Physical therapy will be recommended. In about 4 to 6 months, healing is nearly complete. However, it can take up to a year to return to sports fully.
Prevention
Prevention centers on appropriate daily Achilles stretching and pre-activity warm-up. Maintain a continuous level of activity in your sport or work up gradually to full participation if you have been out of the sport for a period of time. Good overall muscle conditioning helps maintain a healthy tendon.